Skin cancer treatment including skin cancer plastic surgeries require appropriate skill and experience to judge what type of excision , how much dissection is required and type of wound closure for successful functional and aesthetic outcome.
Any one who is dexterous enough can do surgery with proper demonstration and instructions. Nurses we teach can suture and do biopsies or stitching better than the average dermatologist in training .
However, the best surgeon is someone who cares, knows when NOT to operate, knows his-her limits and, is confident with their decisions for the individual patient.
We performs skin surgery and skin cancer surgery daily. We treat skin cancer lesions of any complex shape, size or colour and to any part of the body under local anaesthetic.
Skin lesion and skin cancer treatment/surgery will be tailored to your skin type and overall health, to give you optimal functions and cosmetic outcome. DON’T believe any one who offers scar-less surgery. It’s silly not to expect scaring with any surgery, however, in appropriately experienced hands, the majority of scars will be almost invisible in 3-6 months. Simply use sunscreen to reduce scar line pigmentation.
Don’t waste your money on potions/lotions/snake oils to improve your surgical scars. Let your body heals itself and it’s free ! Some patients will heal faster than others; It’s just a matter of your genetic make up.
Skin cancer treatment can range from simple freezing (cryosurgery) to extensive excision and reconstruction. We tend not to excise and stitch tiny skin cancers ( e.g. 2mm basal cell carcinoma on the back ). Small low risk cancers can be effectively treated with topical medication, freezing or curettage. When done correctly freezing or curettage will give a 98% cure rate. That is the same cure rate as a full excision. These simple methods are great for patients with multiple low risk skin cancers.
Sometimes it is best to leave certain cancers alone and only remove the most trouble ones. Certain skin cancer type will not harm you in the short term. There is no urgency in treating low risk skin cancer (e.g. a slow growing nodular basal cell carcinoma on your back ) when you have other more urgent medical needs to attend to such as a colonoscopy to find out why you are anaemic. Having said that, diagnose and treat your skin cancers while they are small when ever possible.
At times you may be referred to hospital for skin cancer treatment, e.g. one that is overly large and/or has invaded or has grown extremely close to vital structures.
Below are examples of skin cancer treatment/surgeries routinely carried out at our centre. Results will vary between doctors, patients and other factors.
The simplest skin cancer excision is the elliptical excision, an eye shaped piece of skin is removed in order for a nice and neat stitching to occur. Though simple, knowing how to place or orientate the ellipse is just as important as neatness of the incision. First principle is to fully remove the cancer . Cosmetic closure is also of importance.
The majority of our patients, following surgery, return to normal duties the next day. A simple dressing is sufficient.
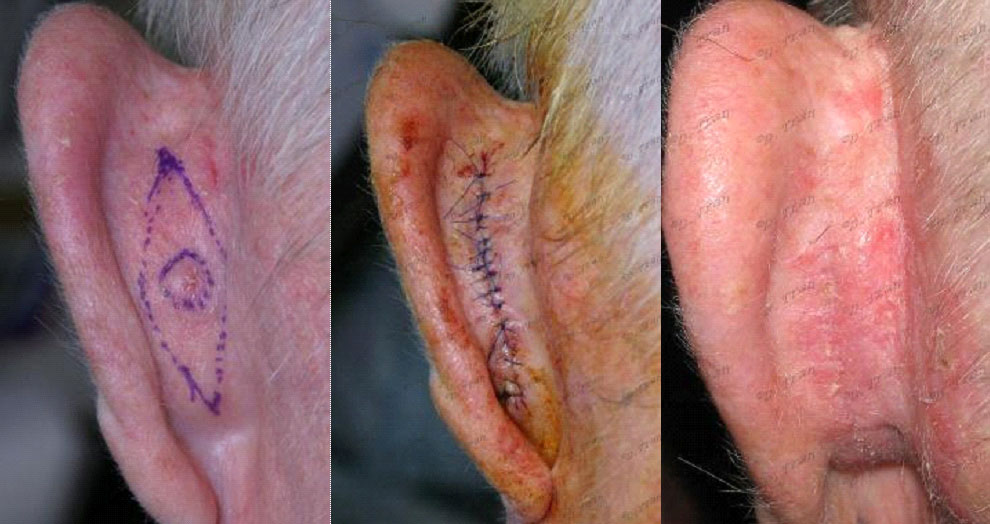
very simple excision of a bcc to the post-auricular groove ( back of the ear )Basal cell carcinoma (Bcc) on the ear. This tumour was excised with a generous outer margins ensuring complete removal in this high risk area. This scar will be barely visible in 3-6 months due to natural scar remodelling process
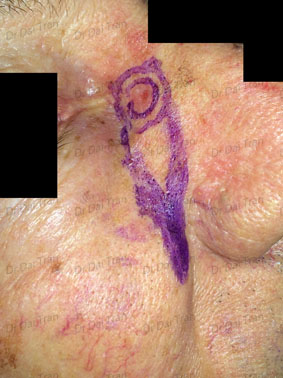
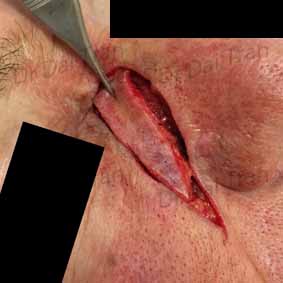
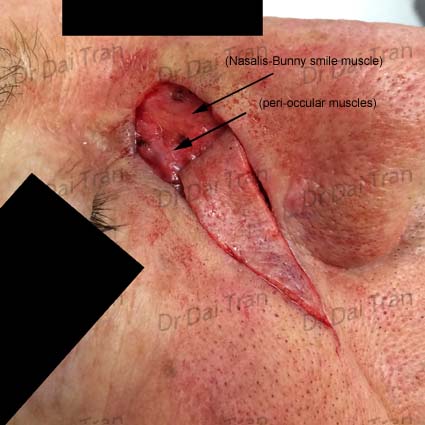
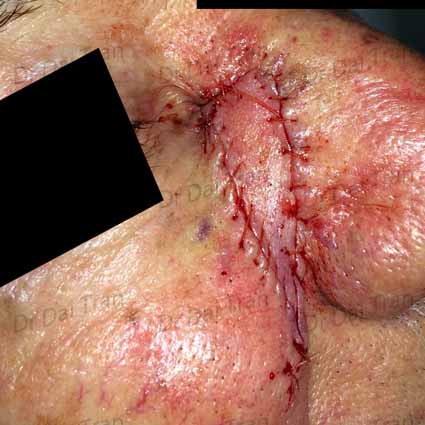
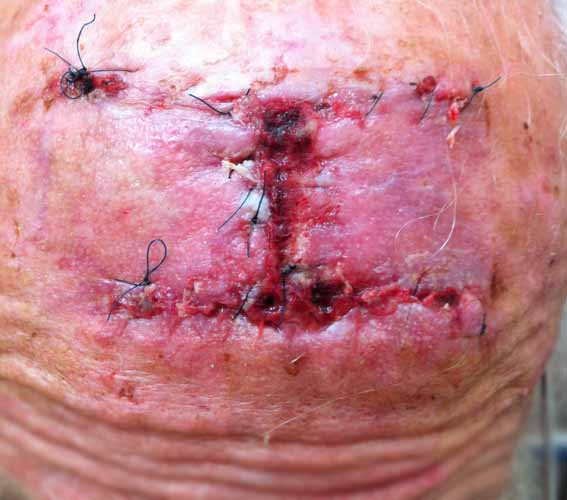
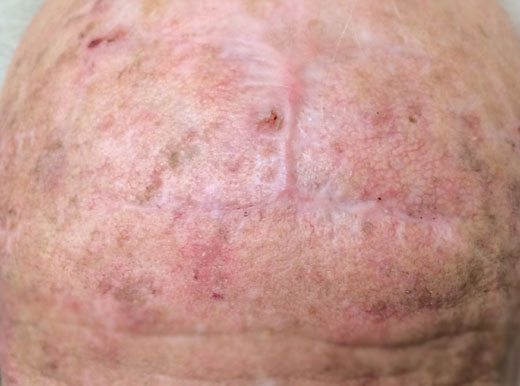
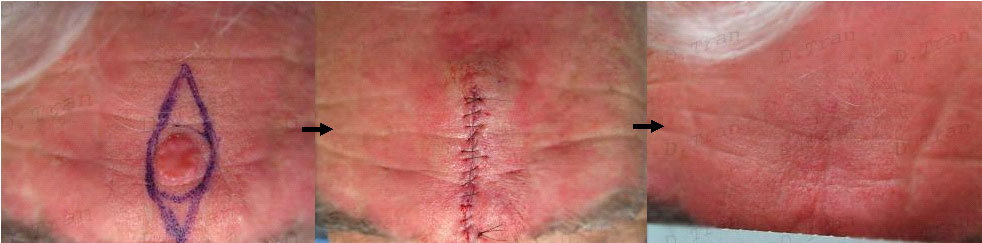 Squamous cell carcinoma on the forehead. This patient had a rapidly growing tumour. To ensure complete removal the incision and dissection was carried out to the muscles and in some case to the periosteum. The wound was closed with absorbable and non absorbable sutures. Sutures were removed 1 weeks post-operatively
Squamous cell carcinoma on the forehead. This patient had a rapidly growing tumour. To ensure complete removal the incision and dissection was carried out to the muscles and in some case to the periosteum. The wound was closed with absorbable and non absorbable sutures. Sutures were removed 1 weeks post-operatively
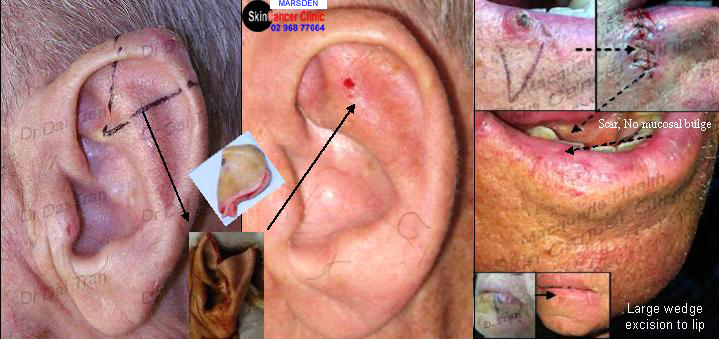
Squamous cell carcinoma to the ear and lip requiring wedge excision. Wedge excision is reserved for the eye-lids, lips and ears. The lip is very elastic, 1/3 of the lip can be wedged out without obvious deformity. The inside surface barely scars. Wedge excision to the ear can be tricky. If done poorly, the wedged scar will spring out leaving a gap defect. A – Z plasty may be needed at times to lock in the wedge. Haematomas can form and they can be dramatic. They must be attended to immediately or cauliflower deformity will develop.
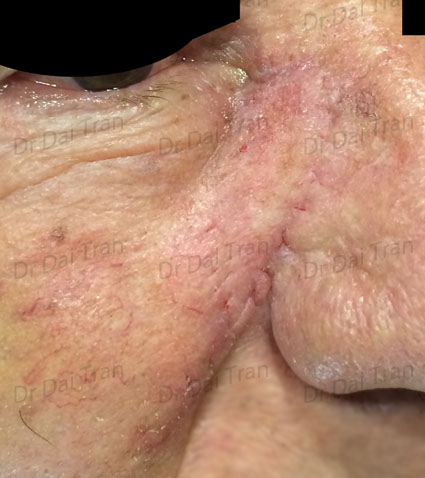
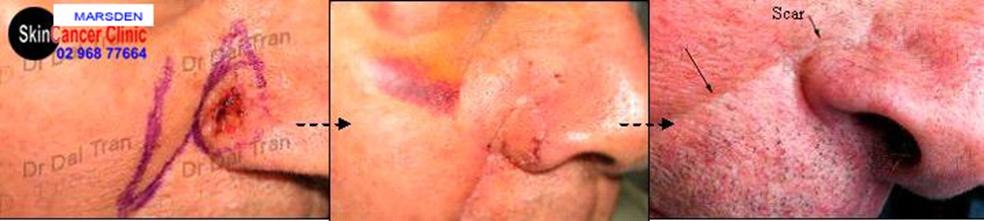
↑skin flap surgery. transpositional flap. Skin is moved from the cheek onto the ala nasi after removing the offending cancer. This flap is tricky even the most entrepreneurial surgeon can give you a nice pin cushion/bumpy displeasing scar afterwards.
When simple wound closure is not possible then skin flap or skin graft surgery is used to repair the surgical wound. Loose skin from adjacent area is moved in to fill the excised defect. Poorly planned skin flap will result in disordered wound contracture and or skin flap necrosis. The worse offending skin flap for poor scaring is the nasal labial transpositional skin flap (see above pictures) . We often see patients with “pin cushion” or “trap door” defects after having surgery done by experience surgeons. Recreating that nostril groove (small arrow) is a real challenge. The scar on the cheek will be invisible… it’s the one on the nose that you should be worried about.
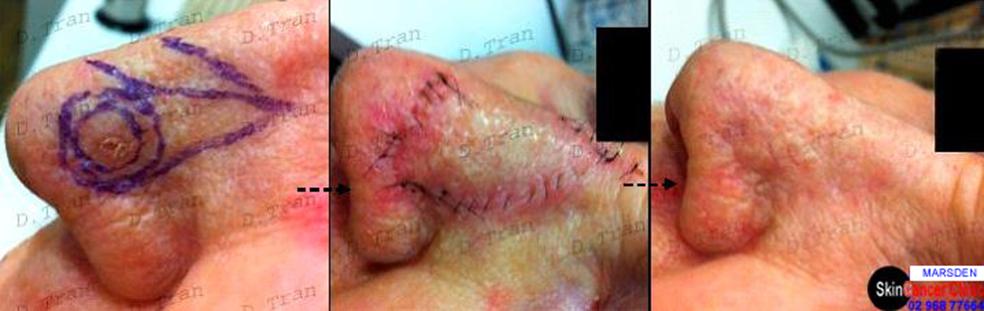
↑Here is example of a more complicated ‘dorsal nasal’ skin flap surgery to treat an awkwardly occurring basal cell carcinoma on the nose. The resulting scar shown was at 12 months postoperative.
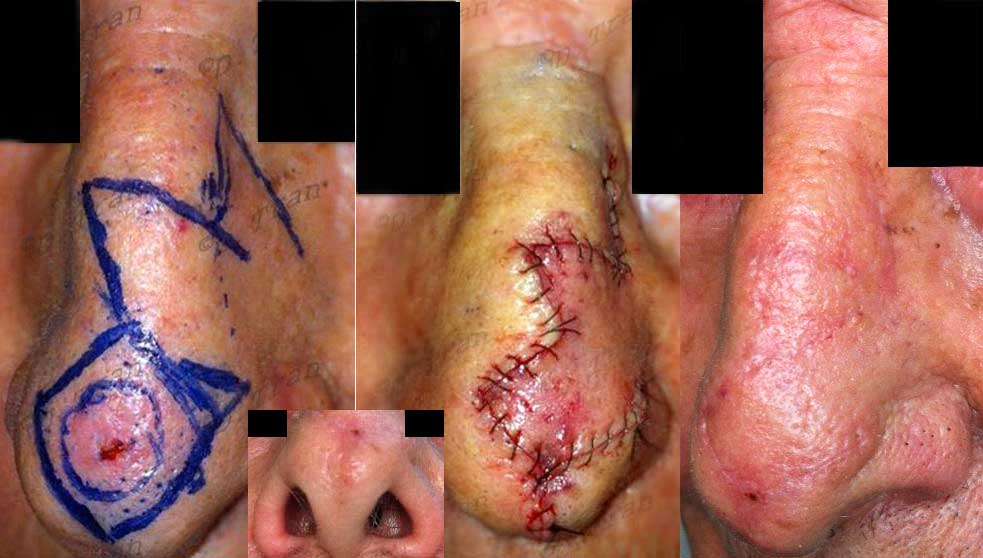
Ulcerated morphoeic basal cell carcinoma to the tip of the nose. Bilobed flap repair. Scar at 14 days post-op. Notice the nostril patency post-op. The nasal valve is well patent.