Skin flap and skin graft surgery
We offer simple to complex skin cancer plastic surgery to everyone. The majority of scars will be almost invisible within 3-6 months.
Use sunscreen to reduce pigmentation to the scar. Don’t waste your time and effort with silico gel, snake oil etc… The natural movement of your skin will naturally remodel the scar for you and, it’s FREE !
The following illustrations were done at the clinic. Results will vary between doctors, patients and other factors.
What is skin flap surgery ?
As the name suggests, a flap of skin is dissected and pulled over to cover the open wound. It takes appropriate experience to judge what type of skin flap and how much dissection is required for successful wound closure. 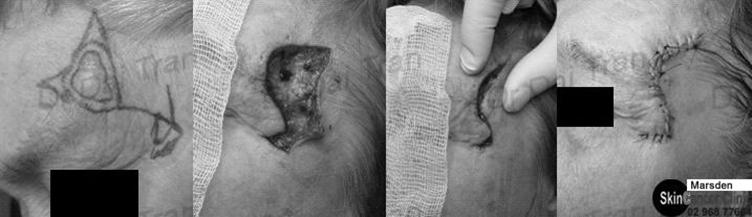
↑In this example, misguided dissection will result in severing of the temporal artery and nerve damage resulting in permanent facial droop.
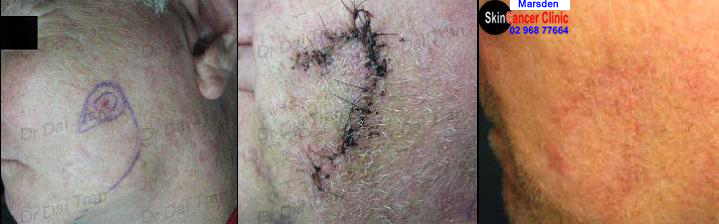 ↑Simple flap ( rotational ) surgery to treat a morphoeic basal cell carcinoma to the cheek. A simple ellipse can be used but, you will end up with an axe-scar
↑Simple flap ( rotational ) surgery to treat a morphoeic basal cell carcinoma to the cheek. A simple ellipse can be used but, you will end up with an axe-scar
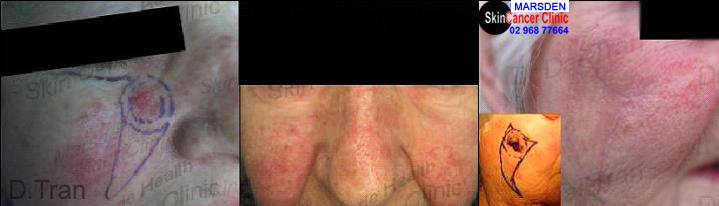
↑Squamous cell carcinoma (left photos). This is a more complicated skin cancer surgery to remove this large mid face tumour. This lateral advancement and rotation skin flap required extensive dissection and many well placed stitches to ensure facial symmetry and avoidance of ectropion ( downward pull of the lower eye lid ). The photos on the right demonstrate a V-Y skin flap surgery to remove a large ulcerated bcc on the outer cheek. Again, extensive dissection and suturing was required. Wound at 1 yr & 1 month
Full thickness skin graft. The cancer is removed. Matching skin is taken from a suitable site e.g. behind the ear. The skin is stitched onto the surgical defect. Cotton dressing (bolster) is tied over the skin graft to press it onto the wound base. Selecting the right donor skin and good suturing will result in a well healed wound. Avoid smoking, strenuous activities and keep the dressing dry to allow the skin graft to heal. Stitches and dressing are removed in 7 to 14 days. Notice: first set of photos, the cancer was removed from the lower eye lid, skin was taken from behind the ear ( 2nd set of photos) and stitched on. Bolster dressing must be kept dry and must not be disturbed. The resulting scar will nice and neat in the majority of cases. Scar should only be judged 3-6 months post-operatively.
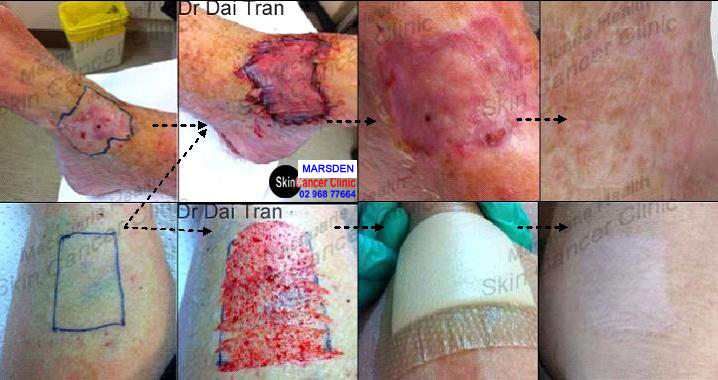
 Split thickness skin grafts surgery are normally reserved for large cancers and on the lower legs. You will require bed rest at home ( with toilet and shower privileges ). The affected leg must be kept elevated, above the shoulders ,for 2 weeks. We therefore, like to keep the graft to 3cm or less. NO SMOKING or the skin graft will die you will be back again for more skin surgery.
Split thickness skin grafts surgery are normally reserved for large cancers and on the lower legs. You will require bed rest at home ( with toilet and shower privileges ). The affected leg must be kept elevated, above the shoulders ,for 2 weeks. We therefore, like to keep the graft to 3cm or less. NO SMOKING or the skin graft will die you will be back again for more skin surgery.
Radiation therapy for skin cancer, is available at various hospitals, Usually reserved for multi-focal cancer, Cancer in awkward areas and for the elderly. The patient will usually be 60 or older. We will prepare your skin ready for Radiation therapy.
Radiation therapy is like going for multiple repeated x-rays. The resulting scar will be fantastic in the short term. Long term the scar will be pale, discoloured and crinkly.
Cryotherapy with liquid nitrogen is the most frequently used method to treat pre-malignant lesions at our clinic. It is quick, simple and effective, BUT, it must be done correctly. The sprayed area will be swollen, blistered, weepy then crusty. Two weeks later, the lesions will peel off leaving behind pink macules. Resulting in the affected skin being slightly paler than the surrounding skin. Cryotherapy is only good for occasional sunspots . For numerous sunspots we prefer “ field therapy “
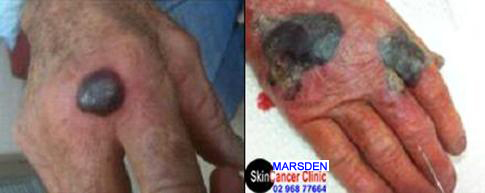
Cryotherapy may cause massive blisters to form. This will usually occur in patients whose skin is very thin and/or taking blood thinners, e.g. asprin, warfarin, etc…You may deflate these large blisters with a large needle but, don’t peel the skin off. Intact skin acts as an excellent biological dressing. WARNING. It is best not to get your skin sprayed before any important photo events ! E.g. parties, unions, weddings etc…
WARNING. Don’t get your skin sprayed before any important photo events ! E.g. parties, unions, weddings etc…
Field therapy with Efudix, Aldara, Picato, Ala…etc should be considered if you have numerous premalignant spots. Treatment is simple. Only the cancerous lesions will be affected. The more pre-cancerous lesions you have the more spotty you will look during the treatment period.
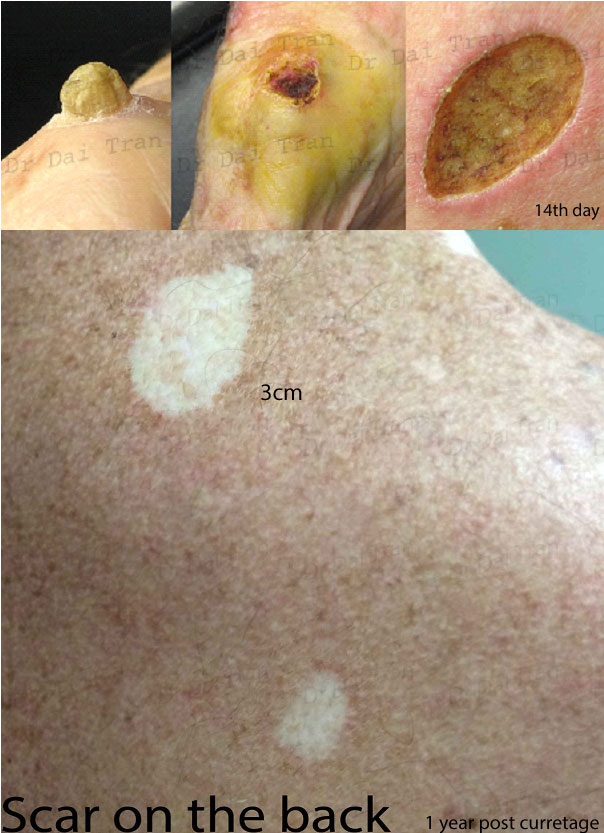
Curettage and cautery, C&C, also known as electrodesiccation and curettage or electrosurgery is a very effective technique for quickly removing low grade skin cancer. However, it is very operator dependent. 98% cure if done correctly. Here a squamous cell carcinoma horn is curreted and cauterized . Wound immediately after cc, at 2 wks, then at ~ 6 months. The resultant white scar can be very obvious on tanned skin.
More examples of the common daily routine surgeries.
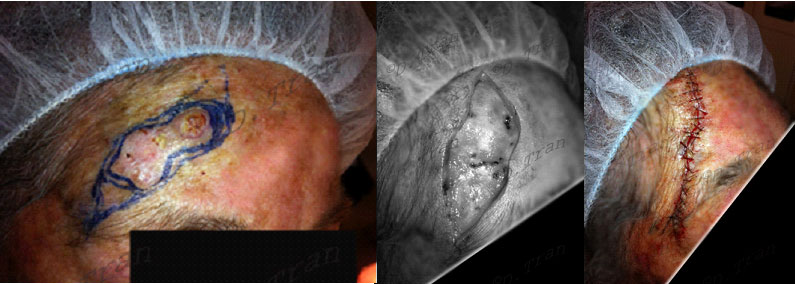
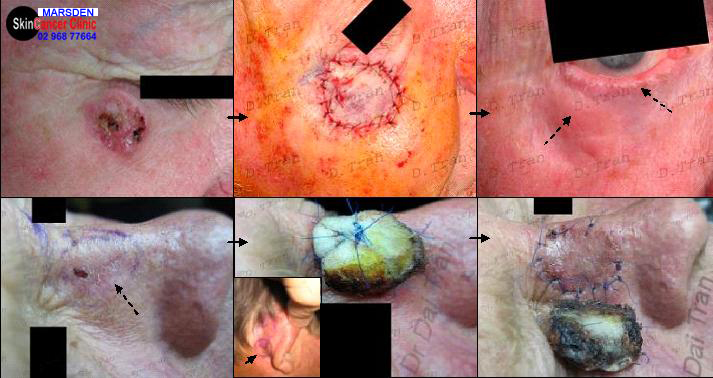
Multifocal squamous cell carcinoma to the temple. Excising large tumors in this location can be a real challenge. The doctor must be a able to deal with significant bleeding, nerve injury and distorted anatomy. For the timid, conservative—minimalist approach will risk incomplete excision of the cancer. Recurrence of cancer in this area can be quite problematic.
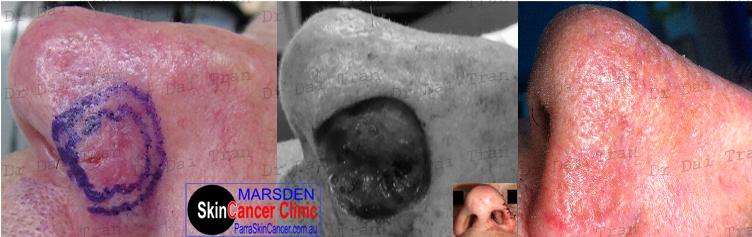
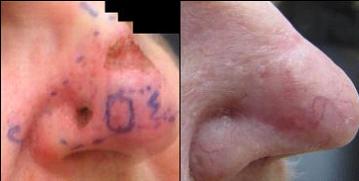
Skin cancer on the nose is very common and so too are recurrences of cancer following skin cancer surgery. Here the infiltrating cancer was excised widely and deeply to cartilage and a full thickness skin graft was used to close the resulting defect. Notice that the nasal valve is widely patent with No obstructing haematoma. Floppy nasal valve can be a real nuisance with breathing, especially with rapid inhalation.
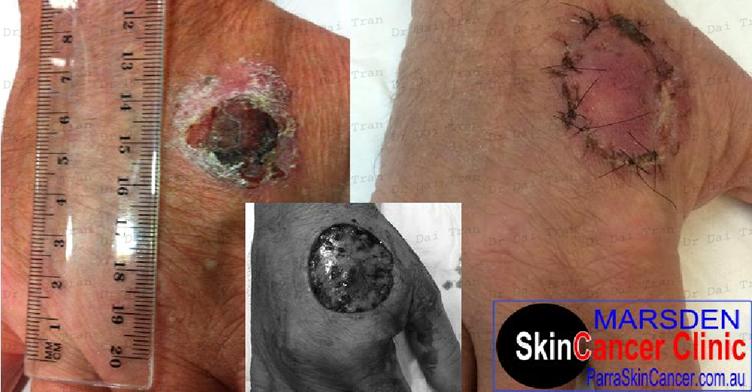
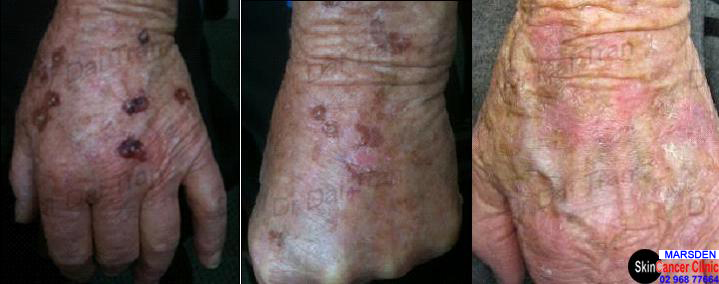
Skin cancer ( squamous cell carcinoma ) to the hand. Excised widely and deeply. Skin grafted. Wound at one week. Squamous cell carcinomas kill more people than melanoma, simply because they are more prevalent but, rest assured—scc on the extremities and esp, those arising from actinic keratosis ( sunspots ) rarely spread unless they are very big. They can be a real pain to treat as they grow very fast.
